Common medications that may increase blood pressure
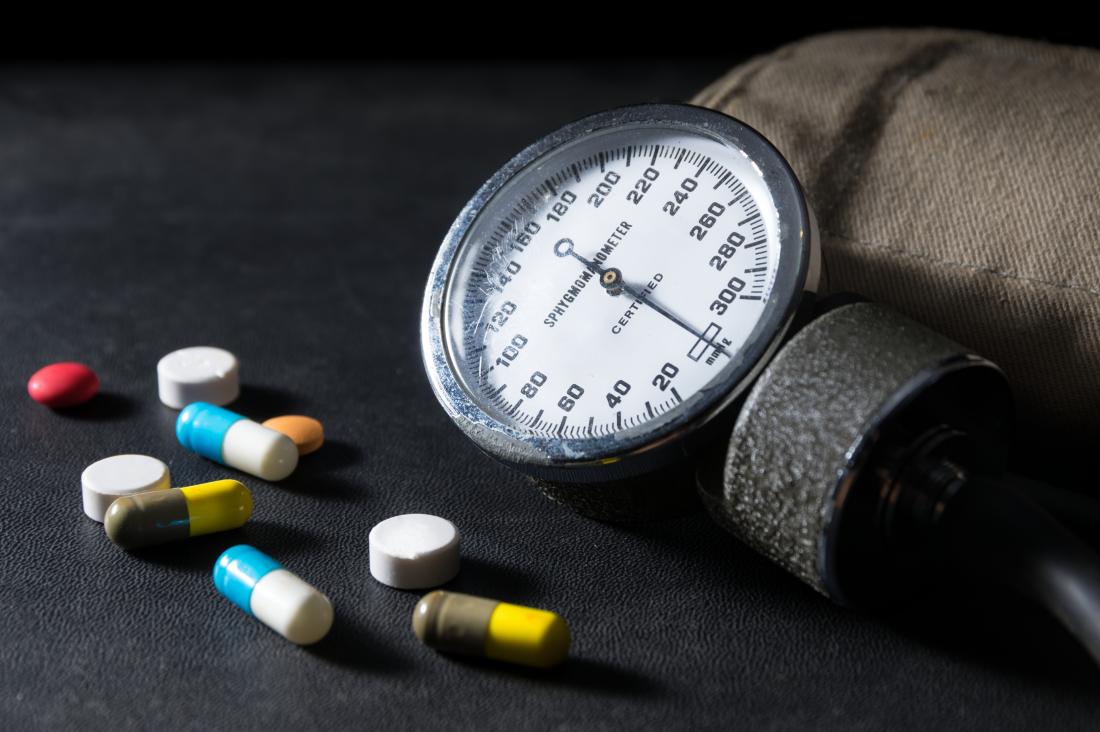
A patient is considered to have high blood pressure when their read out is 140/90mmHg or higher (or 150/90mmHg or higher if they’re over 80). Ideal blood pressure is typically considered to be between 90/60mmHg and 120/80mmHg.
High blood pressure can be down to a wide range of conditions and will need to be managed and monitored effectively. However, certain medications have also been shown to increase blood pressure, for example:
- Steroids
- Non-steroidal anti-inflammatory drugs (NSAIDs) – such as naproxen and ibuprofen
- The contraceptive pill
- Some herbal remedies (especially those containing liquorice)
- Certain recreational drugs including amphetamines and cocaine
- Some over-the-counter cold and flu remedies
- Certain selective serotonin-noradrenaline reuptake inhibitor (SSNRI) antidepressants – such as venlafaxine
Often the patient’s blood pressure will return to normal once they come off the medicine or drug that’s causing it. However, that will obviously need to be balanced against the benefits of taking it in the first place.
Patients at the most risk of high blood pressure
Certain people are more likely to present with high blood pressure than others. Those most at risk are people who:
- Are over 65 years old
- Are overweight or obese
- Lack fruit and vegetables in their diet
- Eat too much salt
- Drink a lot of tea, coffee, alcohol or energy drinks
- Smoke
- Don’t exercise regularly
- Are of black Caribbean or black African descent
- Have a close relative with high blood pressure
- Regularly experience trouble falling asleep or staying asleep
Known causes of high blood pressure
As well as taking certain medications, there are a number of underlying health conditions that are responsible for about 1 in 20 cases of high blood pressure in the UK. These conditions include:
- Diabetes
- Kidney disease
- Long-term kidney infections
- Narrowing of the arteries supplying the kidneys
- Glomerulonephritis (damage to the tiny filters inside the kidneys)
- Obstructive sleep apnoea
- Lupus
- Scleroderma (a condition characterised by thickened skin as well as problems with blood vessels and organs)
- An over or under-active thyroid
- Acromegaly
- Cushing’s syndrome
- Increased levels of the hormone aldosterone (hyperaldosteronism), and phaeochromocytoma
Are you a non-medical prescribing healthcare professional who regularly see patients with hypertension and cardiac failure?
If so, PDUK’s Medicines optimisation in Hypertension and Heart Failure course is well worth considering. Now being offered via Zoom, it’s a great opportunity to gain valuable CPD hours from home.
This flexible and highly interactive programme allows nurses, health visitors and other allied health practitioners to enhance their knowledge in this incredibly diverse area. It looks in detail at important issues non-medical prescribers face regularly, including polypharmacy and patient monitoring. Structured medication reviews are also discussed along with current guidelines.
The course is worth 4 hours of CPD over half a day (10am – 1pm). We’re already seeing plenty of interest though so make sure you book up early to avoid disappointment!